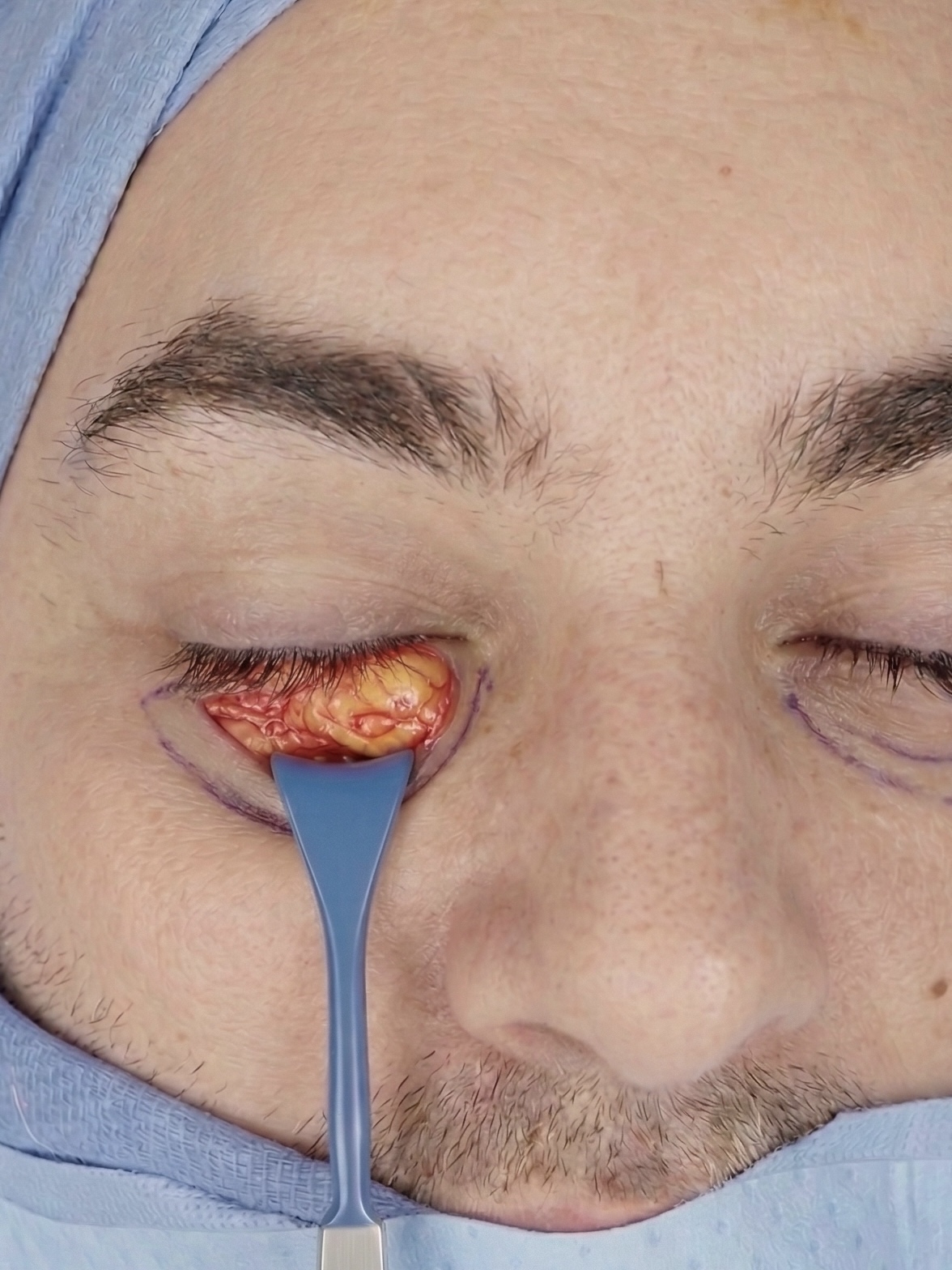
Scarless Transconjunctival Lower Blepharoplasty
This weakening usually happens with age. But bags can also occur in younger patients. This is usually structural – sometimes it is from a smaller orbital cavity that pushes the fat forward, or a flatter cheek that reduces the lower ledge of support beneath the eye. In any case, the fat pads herniate outward, producing a fullness and darkness under the eyes that casts a shadow and reads as tired or aged.
Scarless Blepharoplasty: What That Term Actually Means
Many patients come in already knowing about the transconjunctival incision. Even so, a fair number show signs of surprise when I tell them I plan to go through the inside of the eyelid. There are two fundamentally different ways to perform this surgery, and the approach chosen matters for reasons beyond the visibility of the scar. Avoiding a visible scar is a real advantage, but the primary clinical reason to choose the transconjunctival approach is lower eyelid retraction risk, and that starts with where the incision is made.
So while the phrase “scarless blepharoplasty” has become a popular way of referring to the transconjunctival approach, it is not entirely without nuance. Much like a closed rhinoplasty still involves incisions inside the nose, the conjunctival incision does heal, but it is completely invisible from any external view. The term is accurate in the sense that matters to patients: there is no visible scar on the face.
In a transconjunctival lower blepharoplasty, the lower eyelid is gently pulled down and an incision is made in the pink, wet mucosal lining on the inside. This lining is called the conjunctiva. The next structure encountered is the orbital fat, completely sparing any need to cross the skin or muscle to reach it. With the fat exposed, it can be precisely reduced, or in some cases repositioned, to eliminate the puffiness.
Why the Approach Matters
The most important goal of this surgery is to accomplish the goals of surgery without undue changes to the appearance of the eye. Most notably, lower eyelid retraction, or ectropion.
The lower eyelid is a structurally complex area. Right beneath the very thin skin sits the orbicularis oculi, a circular sphincter muscle. This muscle helps close the eye, and also provides strength to the lid position. Just below that are the fat pads, wrapped in the orbital septum. Approaching the fat through the outer skin requires traversing all three of these layers, creating a full-thickness scar, or thought of another way, a full thickness weakening.
Consider where the lower lid sits, right at the bottom of the eye, with gravity already working against it. Any weakening of the lid’s supportive structures, combined with the downward pull of scar contracture from a full-thickness scar, can pull the lid down. Even just a millimeter of downward shift is visible, bothersome to patients and surgeon alike, and usually a reasonable effort to correct.
The transconjunctival approach avoids a muscular incision entirely. The fat pads are addressed directly through the inside of the eyelid, and the external skin and muscle are never cut. By not creating a full-thickness scar through the skin and muscle, the risk of contracture is reduced, which is exactly why the risk of retraction and ectropion with this approach is substantially lower.
I was trained in both transconjunctival and subciliary approaches, for both cosmetic and reconstructive cases. They each have their applications, and I still use the external approach when it is indicated. But in my experience across a large volume of lid surgery, retraction is significantly lower with the transconjunctival technique, and this is also heavily supported in the medical literature.
A landmark paper by Hamra in Plastic and Reconstructive Surgery drew significant attention to the critical role the orbicularis muscle plays in lower eyelid support. A comparative safety analysis by Korchia et al. confirmed this, showing that bypassing the anterior muscle layer drops the retraction risk to near zero. A split-face study by Netscher et al., where the same patient received a different technique on each eye, found that minor malposition occurred only on the side with the external skin incision, while the transconjunctival side achieved an equivalent cosmetic outcome with no malposition.
What Happens to the Skin
So if you’re not cutting the skin, what happens to it?
Generally, fat herniation acts like a balloon pushing the skin outward, compressing the microvasculature and congesting the area. When the fat is removed, the skin relaxes and redrapes. There can be some minor wrinkling initially as it settles, but in the four to six month postoperative window the skin naturally begins to tighten and improve in tone and texture. These are the long-timeline refinements I discuss with patients that simply are not visible in week one.
It is common that fat grafting is done alongside the scarless blepharoplasty. When fat grafting is added, it redistributes volume to hollow areas, physically volumizing the skin and reducing wrinkling in the process. The added volume can also create a small but structural ledge that strengthens the lower lid position. Lower eyelid laser resurfacing is another effective adjunct. It addresses crepey skin quality that surgery alone would not be expected to resolve, and it can be performed at the same time as surgery or as a separate procedure later. Correcting the volume issues of the lid through fat reduction and grafting decompresses the lower eyelid in a way that inherently improves skin quality once fully healed.
Recovery
Because there is no external incision, the visible signs of surgery after transconjunctival blepharoplasty are primarily swelling and bruising. There is no visible suture line and no external wound to manage. Showering after surgery is entirely fine.
I ask patients to perform gentle massage and stretching exercises of the lids as a safety measure to help the site heal optimally. This is something I am comfortable recommending precisely because there are no delicate external incisions under their fingers. The recovery is more streamlined as a result.
Bruising and swelling are expected, typically peaking around day three to five before beginning to subside. Most patients are socially presentable by ten to fourteen days, and the result continues to refine over the following months as residual swelling resolves. Most patients are wearing sunglasses and running normal errands within the first week.
Who This Isn’t For
Patients with significant under-eye skin excess, poor lower lid tone, or pre-existing lower lid laxity or retraction are not ideal candidates for a transconjunctival-only approach. These patients often require dedicated lid-strengthening procedures at the time of surgery, of which there are several, and an external approach may be the more appropriate fit to allow for that structural reinforcement.
The technique is never selected in advance. It follows from a detailed anatomical exam.